 |
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 22(3); 2017 > Article |
|
Abstract
Purpose
Methods
Results
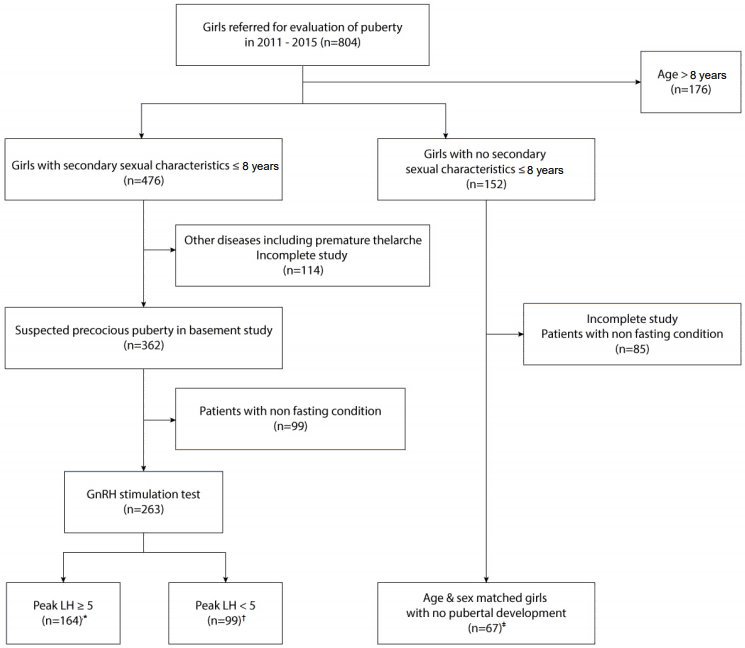
Fig.Ā 1.
TableĀ 1.
| Characteristic | CPP (n=164) | Non-CPP (n=99) | Control (n=67) | P-value* | P-valueā | P-valueā” | Overall P-valueĀ§ |
|---|---|---|---|---|---|---|---|
| CA (yr) | 8.3Ā±0.6 | 8.1Ā±0.8 | 7.9Ā±0.6 | 0.001 | 0.077 | 0.056 | 0.001 |
| BA (yr) | 9.7Ā±0.9 | 9.2Ā±1.0 | 8.2Ā±0.9 | 0.001 | 0.001 | 0.003 | 0.001 |
| BAāCA (yr) | 1.3Ā±0.7 | 1.1Ā±0.7 | 0.0Ā±1.5 | 0.001 | 0.001 | 0.117 | 0.001 |
| Ht. SDS | 0.9Ā±1.1 | 0.8Ā±1.0 | 0.5Ā±0.9 | 0.011 | 0.063 | 0.999 | 0.012 |
| Wt. SDS | 0.7Ā±1.3 | 0.9Ā±1.3 | 0.5Ā±0.9 | 0.714 | 0.142 | 0.782 | 0.138 |
| BMI SDS | 0.3Ā±1.1 | 0.9Ā±1.3 | 0.4Ā±0.9 | 0.999 | 0.633 | 0.237 | 0.195 |
| SHBG (nmol/L) | 80.2Ā±36.7 | 76.5Ā±34.7 | 83.3Ā±31.5 | 0.999 | 0.671 | 0.999 | 0.460 |
| LH0 (IU/L) | 1.1Ā±1.2 | 0.5Ā±0.4 | 0.3Ā±0.3 | 0.001 | 0.615 | 0.001 | 0.001 |
| Peak LH (IU/L) | 12.9Ā±9.5 | 3.2Ā±1.0 | - | - | - | 0.003 | 0.001 |
| Peak LH/LH0 | 23.3Ā±22.7 | 9.3Ā±5.8 | - | - | - | 0.003 | 0.001 |
| E2 (pg/mL) | 12.0Ā±12.5 | 9.5Ā±9.0 | 5.0Ā±0.3 | 0.001 | 0.016 | 0.162 | 0.001 |
| FEI (pmol/L) | 17.8Ā±18.3 | 15.3Ā±17.1 | 7.0Ā±2.7 | 0.001 | 0.004 | 0.675 | 0.001 |
| IGF-1 (ug/L) | 271.6Ā±91.4 | 238.9Ā±70.9 | 220.6Ā±64.3 | 0.001 | 0.463 | 0.005 | 0.001 |
| AST (IU/L) | 27.3Ā±8.9 | 28.6Ā±10.3 | 27.1Ā±5.1 | 0.999 | 0.883 | 0.713 | 0.433 |
| ALT (IU/L) | 14.8Ā±5.7 | 17.5Ā±12.1 | 14.8Ā±6.7 | 0.999 | 0.112 | 0.037 | 0.028 |
| Total cholesterol (mg/dL) | 168.5Ā±28.7 | 164.7Ā±27.2 | 169.4Ā±23.0 | 0.999 | 0.831 | 0.842 | 0.457 |
| Triglycerides (mg/dL) | 116.0Ā±68.6 | 109.5Ā±61.6 | 111.4Ā±58.1 | 0.999 | 0.999 | 0.999 | 0.718 |
| LDL-cholesterol (mg/dL) | 94.6Ā±27.1 | 93.5Ā±26.6 | 95.9Ā±21.8 | 0.999 | 0.999 | 0.999 | 0.850 |
| HDL-cholesterol (mg/dL) | 51.2Ā±10.1 | 50.4Ā±9.9 | 51.8Ā±8.5 | 0.999 | 0.999 | 0.999 | 0.637 |
| Fasting plasma glucose (mg/dL) | 94.7Ā±11.1 | 96.1Ā±11.9 | 91.8Ā±8.1 | 0.204 | 0.035 | 0.864 | 0.040 |
| Insulin (Ī¼U/mL) | 23.5Ā±22.9 | 22.5Ā±26.5 | 12.0Ā±6.8 | 0.001 | 0.008 | 0.999 | 0.001 |
| HOMA-IR | 5.69Ā±5.85 | 5.68Ā±7.37 | 2.78Ā±1.72 | 0.002 | 0.005 | 0.999 | 0.002 |
| QUICKI | 0.32Ā±0.04 | 0.33Ā±0.05 | 0.34Ā±0.04 | 0.003 | 0.194 | 0.390 | 0.004 |
Values are presented as meanĀ±standard deviation.
CPP, central precocious puberty; CA, chronological age; BA, bone age; SDS, standard deviation scores; Ht., height; Wt., weight; BMI, body mass index; SHBG, sex hormone binding globulin; LH, luteinizing hormone; E2, estradiol; FEI, free estradiol index; IGF-1, insulin-like growth factor-1; AST, aspartate aminotransferase; ALT, alanine aminotransferase; LDL, low-density lipoprotein; HDL, high-density lipoprotein; HOMA-IR, homeostasis model assessment-insulin resistance; QUICKI, quantitative insulin sensitivity check index
TableĀ 2.
| Characteristic | BMI<50th %ile (n=87) | 50th %ileā¤BMI<85th %ile (n=57) | BMIā„85th %ile (n=20) | P-value* | P for trendā |
|---|---|---|---|---|---|
| CA (yr) | 8.3Ā±0.6 | 8.4Ā±0.6 | 8.2Ā±0.7 | 0.482 | 0.960 |
| BA (yr) | 9.6Ā±0.9 | 9.6Ā±0.9 | 10.2Ā±1.0 | 0.018 | 0.018 |
| BAāCA (yr) | 1.2Ā±0.7 | 1.2Ā±0.7 | 2.0Ā±0.9 | 0.001 | 0.001 |
| SHBG (nmol/L) | 98.6Ā±34.2 | 66.0Ā±27.2 | 40.7Ā±17.0 | 0.001 | 0.001 |
| LH0 (IU/L) | 1.1Ā±1.3 | 1.1Ā±1.3 | 1.1Ā±0.8 | 0.952 | 0.842 |
| Peak LH (IU/L) | 12.7Ā±9.7 | 13.3Ā±9.2 | 12.5Ā±9.9 | 0.924 | 0.953 |
| E2 (pg/mL) | 13.2Ā±14.1 | 10.3Ā±10.3 | 11.2Ā±9.6 | 0.367 | 0.259 |
| FEI (pmol/L) | 15.0Ā±16.7 | 18.1Ā±18.7 | 29.5Ā±20.1 | 0.007 | 0.004 |
| IGF-1 (ug/L) | 278.4Ā±94.0 | 251.5Ā±87.4 | 298.9Ā±83.5 | 0.081 | 0.950 |
| AST (IU/L) | 26.4Ā±5.7 | 29.6Ā±12.5 | 24.3Ā±6.8 | 0.032 | 0.887 |
| ALT (IU/L) | 12.8Ā±3.4 | 16.1Ā±6.0 | 19.8Ā±8.0 | 0.001 | 0.001 |
| Total cholesterol (mg/dL) | 165.6Ā±25.7 | 174.0Ā±33.2 | 165.2Ā±26.2 | 0.198 | 0.457 |
| Triglycerides (mg/dL) | 108.3Ā±72.8 | 122.4Ā±66.3 | 130.9Ā±53.4 | 0.284 | 0.117 |
| LDL-cholesterol (mg/dL) | 92.8Ā±27.3 | 98.3Ā±26.6 | 92.4Ā±27.6 | 0.457 | 0.630 |
| HDL-cholesterol (mg/dL) | 52.0Ā±10.5 | 51.2Ā±9.6 | 46.9Ā±8.7 | 0.139 | 0.081 |
| Fasting plasma glucose (mg/dL) | 94.3Ā±11.6 | 94.4Ā±11.2 | 96.9Ā±8.1 | 0.647 | 0.461 |
| Insulin (Ī¼U/mL) | 17.2Ā±13.9 | 23.2Ā±22.8 | 51.9Ā±32.8 | 0.001 | 0.001 |
| HOMA-IR | 4.15Ā±3.87 | 5.60Ā±5.79 | 12.60Ā±8.14 | 0.001 | 0.001 |
| QUICKI | 0.33Ā±0.04 | 0.32Ā±0.04 | 0.28Ā±0.02 | 0.001 | 0.001 |
Values are presented as meanĀ±standard deviation.
BMI, body mass index; CPP, central precocious puberty; CA, chronological age; BA, bone age; SHBG, sex hormone binding globulin; LH, luteinizing hormone; E2, estradiol; FEI, free estradiol index; IGF-1, insulin-like growth factor-1; AST, aspartate aminotransferase; ALT, alanine aminotransferase; LDL, low-density lipoprotein; HDL, high-density lipoprotein; HOMA-IR, homeostasis model assessment-insulin resistance; QUICKI, quantitative insulin sensitivity check index.
TableĀ 3.
Insulin resistance is positively correlated with BA advancement, BMI SDS, FEI, IGF-1, and triglycerides and was negatively correlated with SHBG.
HOMA-IR, homeostasis model assessment-insulin resistance; QUICKI, quantitative insulin sensitivity check index; BA, bone age; CA, chronological age; SDS, standard deviation scores; BMI, body mass index; SHBG, sex hormone binding globulin; LH, luteinizing hormone; FEI, free estradiol index; IGF-1, insulin-like growth factor-1; AST, aspartate aminotransferase; ALT, alanine aminotransferase; LDL, lowdensity lipoprotein.
TableĀ 4.
When insulin resistance increased, the odds for BA advancement increased. Model 1 is a multiple logistic regression adjusted for chronological age. Adjusted OR for chronological age and BMI represented in model 2.
HOMA-IR, homeostasis model assessment-insulin resistance; QUICKI, quantitative insulin sensitivity check index; SE Ī², standard error of Ī² coefficient; OR, odds ratio; CI, confidence interval; model 1, adjusted for chronological age (CA); model 2, adjusted for CA and body mass index (BMI).
References
- TOOLS
- Related articles in APEM







