|
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 29(2); 2024 > Article |
|
┬Ę Thyroid eye disease (TED) is an autoimmune disorder with clinical manifestations including lid retraction, proptosis, decreased visual acuity, and strabismus and an incidence rate of 0.79 to 6.5 cases per 100,000 children. This is the first report to describe orbital apex syndrome in pediatric TED, and the presented data will contribute to future analysis of the clinical features of atypical pediatric TED.
To the editor,
Thyroid eye disease (TED) is an immune-mediated inflammatory disease of the eye and orbital tissues. The incidence of TED is 2.9 to 16.0 cases per 100,000 population, which decreases to 0.79 to 6.5 cases per 100,000 of the pediatric population [1,2]. In the present report, we describe a case in which orbital apex syndrome was the initial presentation of TED in an adolescent.
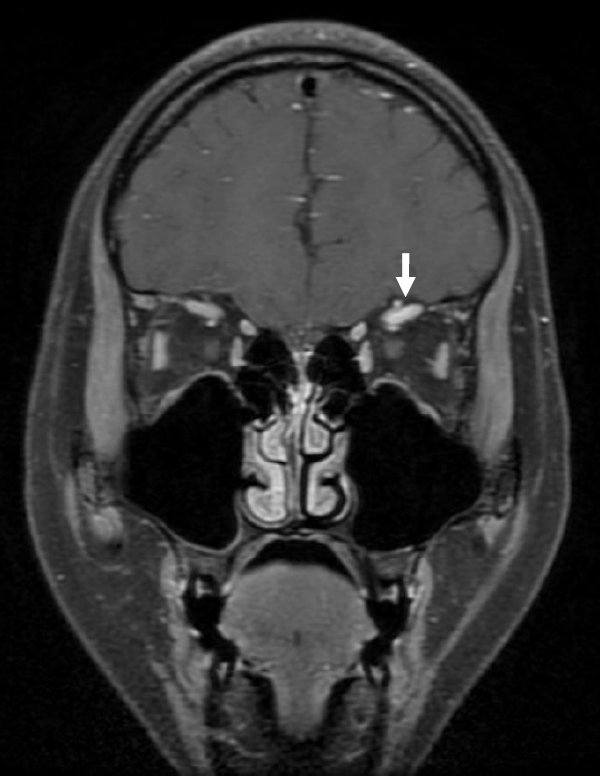
A 17-year-old girl presented with diplopia and hypoesthesia of the left forehead. On examination, hypoesthesia of the left dermatome corresponding to the ophthalmic division of cranial nerve V was detected, in addition to ptosis and edema of the left eyelid. The patient showed decreased visual acuity from previous 20/16 vision to 20/20 vision in both eyes, which is within the normal visual range but relatively poor, as well as restricted ocular movement that prevented upward gaze and left eye abduction (Fig. 1). To evaluate the cause of diplopia and hypoesthesia, thyroid function tests, blood tests, cerebrospinal fluid examination, urine tests, and magnetic resonance imaging (MRI) of the orbital area were performed. Graves' disease was diagnosed on the basis of blood tests: thyroid-stimulating hormone 0.01 ╬╝IU/mL, free thyroxine 4.15 ng/dL, and detection of thyroid-stimulating hormone receptor antibody. Orbital MRI revealed hyperemia and edema of the left superior rectus muscle but no involvement of the tendinous portion (Fig. 2). Therefore, the girl was diagnosed with orbital apex syndrome as the initial presentation of TED owing to decreased visual acuity, restricted ocular movement, and paresthesia of the skin, characterized by involvement of cranial nerves II, III, IV, and VI and the ophthalmic division of cranial nerve V. In addition to the antithyroid agent methimazole, intravenous methylprednisolone pulse therapy was administered for 12 weeks. All symptoms of neuropathy, except mildly reduced visual acuity, improved after 4 weeks of therapy. After 6 months, the patient continues to receive 5 mg (0.1 mg/kg) methimazole and maintains euthyroidism.
Orbital apex syndrome is characterized by reduced visual acuity, restricted ocular movement, and pain or paresthesia of the periorbital skin due to cranial nerve damage or involvement of the orbital apex. The causal factors of orbital apex syndrome include infections, autoimmune diseases, anatomical defects, trauma, and iatrogenicity [3]. Stimulation of orbital fibroblasts induces pathological changes in the extraocular muscles and orbital tissue, causing TED. This leads to the synthesis of glycosaminoglycans and hyaluronic acid, which increases the volume of orbital muscles and tissue through excessive water retention, producing edema [2,4]. These changes can result in cranial nerve compression at the orbital apex, causing orbital apex syndrome. Neuropathic symptoms of TED, such as diplopia and blurred vision, are rare in pediatric patients, whose symptoms are typically mild [5-7]. In 2014, Lim et al. [8] reported a single case of diplopia in 13 pediatric patients diagnosed with TED in Singapore from 2006 to 2012. In 2020, Sim et al. [9] reported a single case of diplopia and blurred vision as neurological symptoms in 19 pediatric patients diagnosed with TED at a separate tertiary care referral center in Singapore between 2006 and 2015. Both studies reported that conservative therapy alone was able to improve the symptoms.
Orbital involvement is typically bilateral. The mechanism of unilateral TED remains unclear, although its incidence increases with age and TED activity, in which asymmetric TED is presumed to develop bilaterally [10]. In 2018, Kim et al. [11] first reported exotropia and hypotropia of the left eye as the initial presentation of pediatric TED in an 18-year-old male. Upon diagnosis, only neurological symptoms, without proptosis or lid abnormalities, were observed. After 3 months of therapy, the diplopia improved, but proptosis in the right eye and bilateral lid retraction developed. Therefore, although neurological symptoms improved after therapy, careful follow-up will be required.
In the absence of specific biochemical markers to diagnose TED, the diagnosis relies on ocular signs and symptoms, thyroid autoimmunity, and exclusion of other diseases [2]. One of the diseases that requires exclusion for diagnosis of TED is idiopathic orbital myositis. In differential diagnosis, imaging results are critical. In general, orbital myositis exhibits a focal or diffuse inflammatory lesion on neuroimaging; muscle and tendon involvement is more irregular. In contrast, in TED, more diffuse and regular ocular muscle involvement is observed, and the tendon is preserved. Hence, radiological findings are important in the diagnosis of TED [12,13]. In our case, although the patient was in a hyperthyroid state, the symptoms were unilateral, and neurological symptoms were more likely to be due to myopathy than neuritis, which necessitated differentiation from orbital myositis. Orbital MRI results indicated regular involvement of the left ocular muscle but no involvement of the tendinous portion. Laboratory findings also suggested active thyroid disease, based on which TED was diagnosed. In pediatric patients, the clinical symptoms of TED can be atypical and diverse, and imaging tools should be appropriately applied to perform the necessary evaluations.
To the best of our knowledge, this is the first report of orbital apex syndrome in a pediatric patient with TED. When orbital apex syndrome occurs in children, the possibility of Graves' disease should be considered; if necessary, steroid treatment should be performed. The present data will contribute to future analyses of atypical TED symptoms.
Notes
References
2. Szczapa-Jagustyn J, Gotz-Wieckowska A, Kociecki J. An update on thyroid-associated ophthalmopathy in children and adolescents. J Pediatr Endocrinol Metab 2016;29:1115ŌĆō22.


4. Kazim M, Goldberg RA, Smith TJ. Insights into the pathogenesis of thyroid-associated orbitopathy: evolving rationale for therapy. Arch Ophthalmol 2002;120:380ŌĆō6.


5. Krassas GE, Gogakos A. Thyroid-associated ophthalmopathy in juvenile Graves' disease--clinical, endocrine and therapeutic aspects. J Pediatr Endocrinol Metab 2006;19:1193ŌĆō206.


6. Goldstein SM, Katowitz WR, Moshang T, Katowitz JA. Pediatric thyroid-associated orbitopathy: the Children's Hospital of Philadelphia experience and literature review. Thyroid 2008;18:997ŌĆō9.


7. Holt H, Hunter DG, Smith J, Dagi LR. Pediatric Graves' ophthalmopathy: the pre- and postpubertal experience. J AAPOS 2008;12:357ŌĆō60.


8. Lim NC, Amrith S, Sundar G. Pediatric thyroid eye disease--the Singapore experience. Orbit 2014;33:96ŌĆō103.


9. Sim B, Chng CL, Audrey C, Seah LL. A retrospective study of pediatric thyroid eye disease: the Asian experience. Orbit 2022;41:69ŌĆō78.


10. Panagiotou G, Perros P. Asymmetric Graves' orbitopathy. Front Endocrinol (Lausanne) 2020;11:611845.



11. Kim WJ, Moon JS, Kim MM. Exotropia and hypotropia as the initial presentation sign of thyroid eye disease in an 18-year-old man. J AAPOS 2018;22:71ŌĆō3.


12. ERÛZ P, Argin MA. Recurrent idiopathic orbital myositis: two case reports. Int J Ophthalmol Clin Res 2019;6:110.