 |
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 27(4); 2022 > Article |
|
Abstract
Purpose
Methods
Results
Notes
Funding
This study was partially supported by a grant from the Korea Institute of Radiological and Medical Sciences (KIRAMS), funded by the Ministry of Science and ICT (MSIT), Republic of Korea. (No.50541-2019).
Fig.┬Ā1.
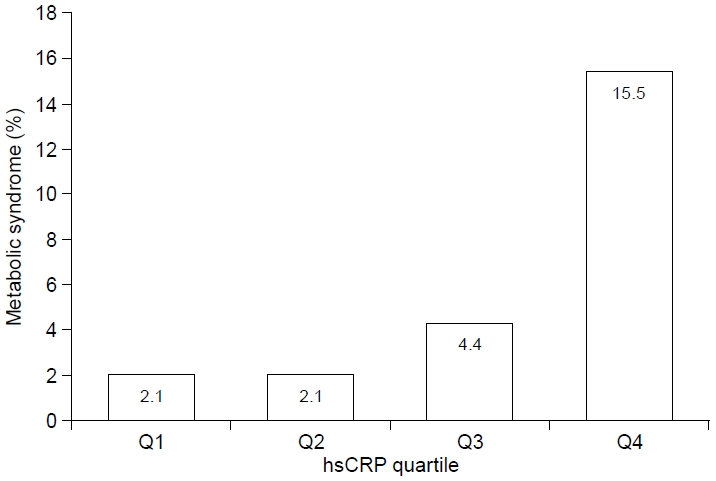
Fig.┬Ā2.

Table┬Ā1.
Values are presented as mean┬▒standard deviation.
MetS, metabolic syndrome; hsCRP, high-sensitivity C-reactive protein; BMI, body mass index; WC, waist circumference; SBP, systolic blood pressure; DBP, diastolic blood pressure; FPG, fasting plasma glucose; TG, triglyceride; HDL-C, high-density lipoprotein cholesterol; HbA1c, glycosylated hemoglobin; TC, total cholesterol; LDL-C, low-density lipoprotein cholesterol.
Metabolic syndrome is defined as at least 3 of the following 5 criteria: WC Ōēź90th percentile, SBP or DBP Ōēź90th percentile, FPG Ōēź100 mg/dL, TG Ōēź110 mg/dL, and HDL-C Ōēż40 mg/dL.
Table┬Ā2.
| Variable |
Quartiles of hsCRP (mg/dL)ŌĆĀ |
P-value | |||
|---|---|---|---|---|---|
| Q1 (<0.27) | Q2 (0.27ŌĆō0.37) | Q3 (0.37ŌĆō0.70) | Q4 (Ōēź0.70) | ||
| Number | 284 | 330 | 317 | 316 | |
| Metabolic syndrome (%) | 2.1 | 2.1 | 4.4 | 15.5 | <0.001 |
| Abdominal obesity (%) | 3.5 | 3.3 | 9.1 | 31.3 | <0.001 |
| High blood pressure (%) | 7.4 | 11.5 | 15.8 | 22.8 | <0.001 |
| Hyperglycemia (%) | 9.5 | 12.4 | 12.6 | 13.6 | 0.461 |
| Hypertriglyceridemia (%) | 19.4 | 15.8 | 20.8 | 28.8 | 0.001 |
| Low HDL-C (%) | 6.0 | 7.6 | 12.3 | 19.0 | <0.001 |
| HbA1c Ōēź5.7 % (%) | 6.3 | 8.3 | 8.0 | 15.0 | 0.001 |
| LDL Ōēź130 mg/dL (%) | 9.2 | 5.8 | 8.5 | 9.2 | 0.331 |
| No. of MetS components | 0.46┬▒0.74 | 0.51┬▒0.79 | 0.71┬▒0.88 | 1.16┬▒1.22 | <0.001 |
Table┬Ā3.
hsCRP, high-sensitivity C-reactive protein; MetS, metabolic syndrome; HDL-C, high-density lipoprotein cholesterol; HbA1c, glycosylated hemoglobin; LDL-C, low-density lipoprotein cholesterol.
Model 1, adjusted for age and sex; Model 2, adjusted for age, sex, and other components of the metabolic syndrome.
Model 2ŌĆĀ in analysis for HbA1cŌēź5.7, adjusted for age, sex, abdominal obesity, high blood pressure, hypertriglyceridemia, and low HDL-C.
References
- TOOLS
- Related articles in APEM







