 |
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 28(4); 2023 > Article |
|
Abstract
Purpose
Methods
Results
Supplementary material
Supplementary Table 1.
Supplementary Table 2.
Supplementary Table 3.
Supplementary Fig. 1.
Notes
Funding
This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Fig. 1.
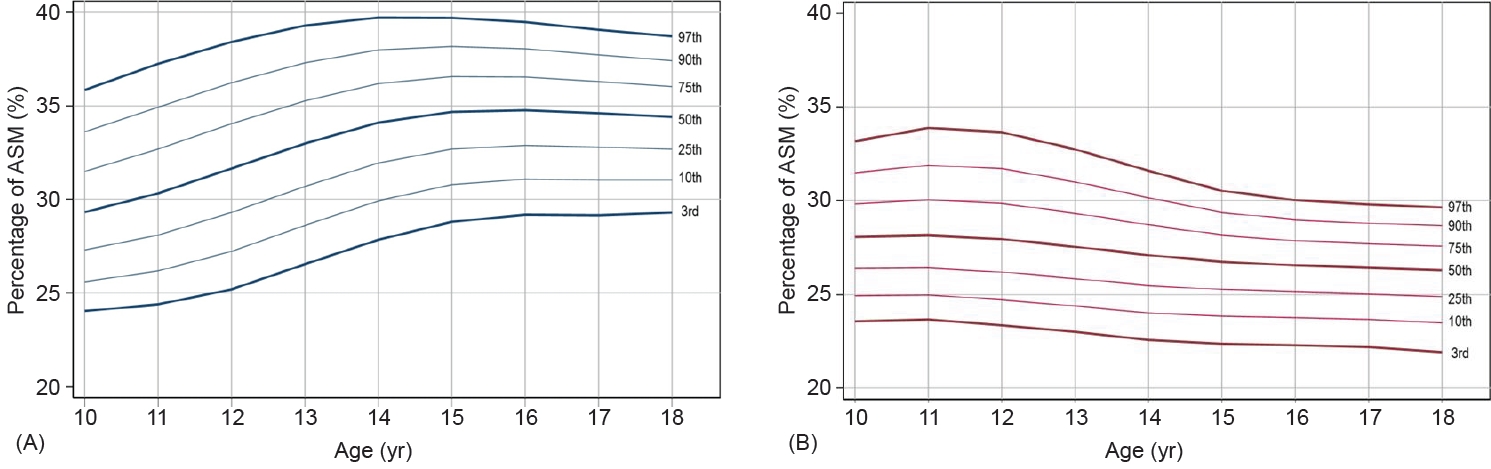
Fig. 2.
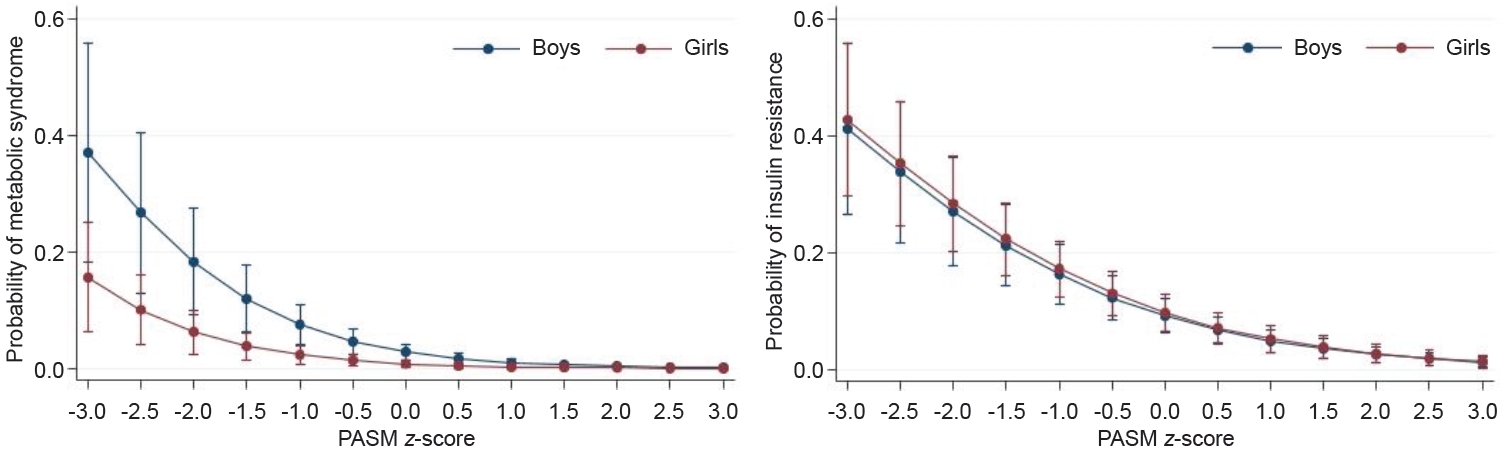
Table 1.
Table 2.
| Variable | Total | Boys | Girls | P-value |
|---|---|---|---|---|
| No. (%) | 1,174 | 613 (52.7) | 561 (47.3) | |
| Age (yr) | 13.9Âą0.1 | 13.9Âą0.1 | 13.9Âą0.1 | 0.888 |
| Height (cm) | 161.1Âą0.4 | 164.8Âą0.6 | 157.0Âą0.4 | <0.001 |
| Weight (kg) | 54.3Âą0.5 | 57.7Âą0.7 | 50.4Âą0.6 | <0.001 |
| BMI z-score | -0.04Âą0.04 | -0.04Âą0.06 | -0.04Âą0.06 | 0.959 |
| BMI category | 0.226 | |||
| âNormal | 935 (79.6) | 479 (78.1) | 456 (81.3) | |
| âOverweight | 127 (10.8) | 67 (10.9) | 60 (10.7) | |
| âObesity | 112 (9.5) | 67 (10.9) | 45 (8.0) | |
| âHousehold income (quintile) | 0.111 | |||
| ââ1Q, lowest | 160 (13.6) | 79 (12.9) | 81 (14.4) | |
| ââ2Q | 254 (21.6) | 125 (20.4) | 129 (23.0) | |
| ââ3Q | 271 (23.1) | 131 (21.4) | 140 (25.0) | |
| ââ4Q | 237 (20.2) | 132 (21.5) | 105 (18.7) | |
| ââ5Q, highest | 252 (21.5) | 146 (23.8) | 106 (18.9) | |
| Daily energy intake (kcal) | 2,083.1Âą30.8 | 2,311.2Âą41.8 | 1,829.1Âą39.5 | <0.001 |
| ASM (kg)â | 15.7Âą0.2 | 18.3Âą0.2 | 13.2Âą0.1 | <0.001 |
| PASM (%)â | 29.8Âą0.2 | 32.8Âą0.2 | 26.9Âą0.2 | <0.001 |
| PASM z-score | -0.02Âą0.05 | 0.09Âą0.06 | -0.14Âą0.07 | 0.005 |
| Fat mass (kg) | 14.9Âą0.2 | 13.7Âą0.3 | 16.4Âą0.3 | <0.001 |
| WC (cm) | 67.4Âą0.3 | 68.3Âą0.4 | 66.3Âą0.4 | <0.001 |
| Systolic BP (mmHg) | 107.5Âą0.4 | 116.1Âą0.5 | 104.6Âą0.5 | <0.001 |
| Diastolic BP (mmHg) | 67.1Âą0.3 | 68.0Âą0.4 | 66.1Âą0.4 | <0.001 |
| Triglyceride (mg/dL)â | 76.6Âą1.7 | 76.3Âą2.4 | 77.0Âą1.8 | 0.792 |
| HDL-C (mg/dL)â | 48.1Âą0.4 | 46.6Âą0.4 | 49.7Âą0.5 | <0.001 |
| LDL-C (mg/dL)â | 88.6Âą0.9 | 84.6Âą1.2 | 93.2Âą1.1 | <0.001 |
| FPG (mg/dL)â | 88.7Âą0.2 | 89.3Âą0.3 | 88.0Âą0.3 | 0.001 |
| Insulin (mIU/L)â | 12.4Âą0.2 | 12.2Âą0.3 | 12.7Âą0.3 | 0.169 |
| Metabolic syndrome | 57 (4.9) | 36 (5.9) | 21 (3.7) | 0.090 |
| Insulin resistance | 185 (15.8) | 91 (14.9) | 94 (16.8) | 0.369 |
| PsiMS | 4.17Âą0.02 | 4.19Âą0.02 | 4.16Âą0.02 | 0.181 |
| HOMA-IRâ | 2.72Âą0.04 | 2.68Âą0.06 | 2.75Âą0.06 | 0.398 |
| TyG indexâ | 8.11Âą0.02 | 8.11Âą0.03 | 8.11Âą0.02 | 0.971 |
Values are presented as weighted meanÂąstandard error or as number (%).
BMI, body mass index; Q, quintile; ASM, appendicular skeletal muscle mass; PASM, percentage of appendicular skeletal muscle mass; WC, waist circumference; BP, blood pressure; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; FPG, fasting plasma glucose; PsiMS, pediatric simple metabolic syndrome score; HOMA-IR, the homeostasis model assessment of insulin resistance; TyG index, triglyceride glucose index.
Overweight is defined as BMI 85thâ¤95th percentile for age and sex, obesity is defined as BMI âĽ95th percentile for age and sex.
Table 3.
References
- TOOLS
-
METRICS

-
- 1 Crossref
- Scopus
- 2,069 View
- 133 Download
- Related articles in APEM






