Single random measurement of urinary gonadotropin concentration for screening and monitoring girls with central precocious puberty
Article information
Abstract
Purpose
The gold standard for assessing pubertal activation is the gonadotropinreleasing hormone (GnRH) stimulation test (GnRHST), which is invasive, time-consuming, and inconvenient. This study evaluated whether a single random measurement of urinary luteinizing hormone (LH) concentration could substitute for the GnRHST in diagnosing and monitoring central precocious puberty (CPP) in girls.
Methods
Fifty-five girls with breast buds before 8 years of age were assessed by both the GnRHST and urinary gonadotropin assays. Based on the GnRHST results, 29 girls were assigned to the CPP group (peak LH≥5 IU/L), and 26 were placed in the premature thelarche (PT) group (peak LH<5 IU/L). Auxological data and urine and serum samples were collected at baseline and after treatment with a GnRH agonist for 12 and 24 weeks.
Results
Although the auxological data did not differ between the 2 groups, the serum levels of insulin-like growth factor-1, basal LH, follicle-stimulating hormone (FSH), estradiol, and peak LH; urinary LH; and peak serum LH/FSH and urinary LH/FSH ratios were higher in the CPP group than in the PT group. Pearson correlation analysis showed a positive correlation between the urinary and serum LH concentrations (r=0.660, P<0.001). Receiver-operating characteristic curve analyses showed that a urinary LH concentration of 0.725 IU/L was a cutoff that significantly predicted positivity on the GnRHST. Urinary LH and FSH concentrations declined significantly during GnRH agonist treatment.
Conclusions
A single, random measurement of urinary gonadotropin concentration could be a reliable tool for initial screening and therapeutic monitoring of CPP in girls.
Highlights
· There are positive correlations between serum gonadotropins and urine gonadotropins.
· Urinary gonadotropin levels reflected the H-P-G axis status in girls with CPP.
· Single, random urinary measurements of gonadotropin concentrations are noninvasive, convenient method for CPP patients.
Introduction
The initiation of puberty requires an increase in the pulsatile release of gonadotropin-releasing hormone (GnRH) from the hypothalamus, which activates pulse generation of luteinizing hormone (LH) and follicle-stimulating hormone (FSH) in the anterior pituitary [1,2]. This is followed by gonadal growth, sex steroid production, and gametogenesis [3,4]. Because the concentrations of LH and FSH increase from 50- to 100-fold and about 10-fold, respectively, between childhood and adulthood, the serum concentrations of basal gonadotropins, especially LH, can reflect pubertal development [5]. However, radioimmunoassay measurements of basal gonadotropin concentrations are inaccurate because some concentrations are below the detectable limit and the levels of those hormones vary diurnally during the prepubertal and early pubertal periods.
Precocious puberty (PP) is historically defined as the onset of developmental signs of sexual maturation before age 8 years in girls and 9 years in boys [6]. The 3 major subtypes of PP are central PP (CPP), peripheral PP, and benign pubertal variants, such as premature thelarche (PT), premature adrenarche, premature pubarche, and gynecomastia [2]. The most common form, CPP, is caused by premature maturation of the hypothalamic-pituitary-gonadal (HPG) axis [6].
The GnRH stimulation test (GnRHST) is considered the gold standard for identifying pubertal activation of the HPG axis and diagnosing CPP. GnRH agonists (GnRHa), which suppress the HPG axis, have been shown to be effective and safe treatments for CPP patients [2,7]. The therapeutic effects of GnRHa can be monitored by measuring gonadotropin responses using the GnRHST. However, performance of the GnRHST involves a long stay in a hospital and repeated blood sampling by venipuncture. Because this testing is expensive, invasive, and inconvenient for children showing early signs of puberty, studies have evaluated methods that could replace or simplify the standard GnRHST [5,8,9].
Recent technological improvements in hormone assays have increased interest in using urine or saliva samples to assess human pituitary function. The collection and analysis of urine samples is more convenient and better tolerated than blood sampling in populations such as neonates and children with needle phobia and for long-term studies. Urinary gonadotropin concentrations have been shown to distinguish among pubertal stages [10,11]. For example, LH concentrations in the first morning-voided (FMV) urine and in 24-hour urine have been shown to correlate with the basal serum LH concentration [5,12]. In addition, CPP can be assessed and monitored by measuring the LH concentration and LH/FSH ratio in FMV urine samples. However, FMV urine sampling and 24-hour urine collection are also inconvenient in outpatient settings.
To determine whether measuring the gonadotropin concentration in a single, random urinary sample can be used as an initial screen for diagnosing CPP and monitoring the treatment response in girls with CPP, we compared the concentrations of urinary gonadotropins and with the basal and peak serum gonadotropins in girls with CPP and PT.
Materials and methods
1. Participants
Girls showing signs of early puberty who had already undergone both the GnRHST and urinary gonadotropin assays were recruited from the growth clinic in the Department of Pediatrics, Chungnam National University Hospital, between August 2017 and July 2018. CPP was defined as breast budding as a first sign of puberty before 8 years of age accompanied by an at least 1-year greater bone age than chronological age and a peak LH level≥5.0 IU/L during the rapid-acting GnRHST (0.1 mg Relefact LHRH; Sanofi-Aventis, Frankfurt am Main, Germany). PT was defined as a peak LH<5.0 IU/L in the GnRHST. Subjects were excluded if they had an underlying disorder or history of medication associated with altered pubertal timing or gonadal development, such as steroids, growth hormone, or GnRHa, or if they were found to have an abnormality on brain MRI or pelvis sonography.
2. Study design
The age, height, weight, body mass index (BMI), parental height, pubertal status, bone age, thyroid function, concentrations of insulin-like growth factor-1 (IGF-1) and estradiol, and medical history were collected from the patients’ medical records. The standard deviations (SDs) for height, weight, and BMI were calculated using the 2017 growth reference for Korean children and adolescents [13]. Venous blood and random urine samples were obtained from all participants before and 15, 30, 45, 60, and 90 minutes after GnRH injection. Blood and urine samples were also collected from girls with CPP after 3 and 6 injections of GnRHa (50–100 μg/kg, leuprolide acetate; Takeda, Osaka, Japan).
3. Gonadotropin analysis
The concentrations of serum and urinary LH and FSH were measured using a 2-site sandwich immunoassay involving a direct chemiluminometric technique on an ADVIA Centaur instrument (Siemens Healthcare Diagnostics Inc., New York, NY, USA). The LH assay had a range of 0.07–200 mIU/mL, with an interassay correlation coefficient of 0.99 and a total coefficient of variation (CV) of 2.7%–3.8%. The FSH assay had a range of 0.3–200 mIU/mL, an interassay correlation coefficient of 0.99, and a total CV of 2.2%–3.9%.
4. Statistics
Continuous variables are presented as mean±SD. The presence of a normal distribution was determined using the Kolmogorov–Smirnov and Shapiro-Wilk tests. The means of auxological and clinical laboratory data in the CPP and PT groups were compared using independent t-tests. Relationships between serum and urinary variables and positive results on the GnRHST were determined using Pearson bivariate correlation, receiver-operating characteristic (ROC) curve, and logistic regression analyses. Associations between the serum and urinary LH concentrations were evaluated using a linear regression analysis. Mean serum and urinary LH levels in response to GnRHa treatment were compared using paired-sample t-tests. Graphs were drawn using GraphPad Prism 6 (GraphPad Software Inc., San Diego, CA, USA). Data were analyzed using IBM SPSS Statistics ver. 22.0 (IBM Co., Armonk, NY, USA), with P<0.05 considered statistically significant.
Results
1. Clinical and laboratory characteristics
Of the 55 girls who showed signs of early puberty and had undergone both the GnRHST and urinary gonadotropin assays, 29 were assigned to the CPP group (peak LH≥ 5 IU/L) and 26 to the PT group (peak LH<5 IU/L). Their anthropometric and laboratory characteristics are summarized in Table 1. Age, height, weight, parental height, predicted adult height, bone age, Tanner stage, and urinary gonadotropin/creatinine (Cr) ratio did not differ significantly between the 2 groups. However, IGF-1, estradiol, basal serum LH and FSH, and peak serum LH concentrations were significantly higher in the CPP group than in the PT group (P<0.05 each). In addition, the peak serum LH/FSH ratio in the GnRHST and basal urinary LH and LH/FSH ratio were significantly higher in the CPP group (P<0.05 each).
2. Association between serum gonadotropin and urinary gonadotropin levels
The associations between pairs of urinary variables and serum variables obtained in the GnRHST were calculated using a Pearson bivariate correlation analysis (Table 2). The urinary LH concentration correlated strongly and positively with the urinary LH/FSH ratio (r=0.884, P<0.001, data not shown), basal serum LH (r=0.660, P<0.001) and FSH (r=0.618, P<0.001) levels, the urinary FSH level (r=0.523, P<0.001), peak serum LH level (r=0.280, P=0.017), peak serum LH/FSH ratio (r=0.471, P=0.001, not shown), and IGF-1 level (r=0.295, P=0.044, data not shown). The urinary LH concentration did not, however, correlate significantly with the peak serum FSH level (r=0.168, P=0.255).
3. Urinary gonadotropin levels as predictors of positive GnRHST
To determine whether measuring the urinary LH level can be used to diagnose CPP, ROC curves were drawn, and the areas under the curves (AUCs) were calculated (Table 3). The AUCs for urinary LH (0.721±0.077, P=0.010) and serum LH (0.749±0.072, P=0.003) concentrations for a positive GnRHST result (peak LH≥5.0 IU/L) were similar. The peak serum LH/FSH ratio had the highest sensitivity and specificity for diagnosing CPP (0.958±0.030, P<0.001), and the urinary LH/FSH ratio was also significant (0.731±0.075, P=0.007). The cutoff urinary LH level for a positive GnRHST was 0.725 IU/L (65.4% sensitivity and 63.6% specificity), which represented a 4-fold improvement in the prediction of a positive GnRHST (odds ratio, 4.048; 95% confidence interval, 1.210–13.538; P=0.023) in a logistic regression analysis. The cutoff for the urinary LH/FSH ratio was 0.057, which had a sensitivity of 65.4% and a specificity of 68.2% (Fig. 1).

Area under the receiver-operating characteristic curve for a positive gonadotropin-releasing hormone stimulation test
4. Changes in urinary gonadotropin levels in girls with CPP after treatment with GnRHa
Girls with CPP who were treated with GnRHa for 12 and 24 weeks saw significant reductions from baseline in their serum and urinary LH and FSH concentrations (Fig. 2).
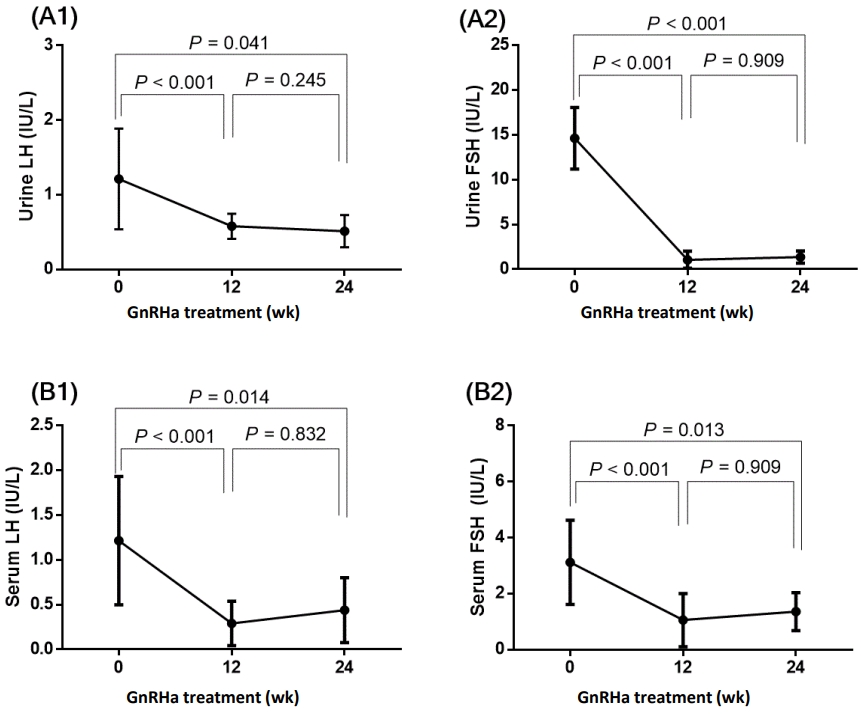
Changes in serum and urinary gonadotropin levels in girls with CPP before and after treatment with GnRHa. (A1) Urinary LH level, (A2) urinary FSH level. (B1) serum LH level, and (B2) serum FSH level. Values are presented as mean±standard deviation. CPP, central precocious puberty, GnRHa: gonadotropin-releasing hormone agonist; LH, luteinizing hormone; FSH, follicle-stimulating hormone.
Discussion
Urinary concentrations of gonadotropins can be easily, noninvasively, and conveniently measured, which could make them a good substitute for a positive GnRHST in diagnosing girls with CPP. In this study, we found that randomly measured urinary concentrations of gonadotropins correlated strongly with the serum concentrations of gonadotropins and that urinary gonadotropins were predictive of a positive GnRHST. Thus, this method could be useful for monitoring girls with CPP during GnRHa treatment.
Although the GnRHST is the gold standard test for diagnosing CPP, it is time-consuming, expensive, invasive, and labor intensive for both patients and physicians in outpatient clinics. Previous studies have sought methods to reduce the discomfort and improve the convenience of diagnosing CPP. One study tested the efficacy of using a single unstimulated LH measurement of ≥0.83 IU/L as a diagnosis of CPP, but that study did not test the efficacy of the LH/FSH ratio [14]. However, both those assays share the limitation that basal serum gonadotropin levels can overlap between prepubertal and pubertal children [15]. A single blood sample obtained 40 minutes after injection of GnRH (gonadorelin) was found to be useful in diagnosing CPP, with 98% sensitivity and 100% specificity, whereas a sample obtained 20 minutes after the injection was useful in assessing pubertal suppression, with 100% sensitivity and specificity [16]. A simplified GnRHST involving a single sample obtained 30 minutes after a GnRH injection was found to be useful in diagnosing CPP and assessing its suppression [17,18]. Because the unstimulated serum LH levels in this study accounted for only 74.9% of the positivity in the test for CPP, a single measurement of the basal serum LH concentration might be better used as an initial screening for puberty onset rather than as a replacement for the GnRHST when diagnosing CPP.
Compared with blood sampling, urine sampling is convenient, painless, and more tolerable for young patients. In the 1960s, scientists first detected the urinary excretion of LH and FSH in adults and reported the usefulness of urine samples in differentiating sex hormone disorders [19,20]. Ultrasensitive liquid chromatography–tandem mass spectrometry-based steroid assays can detect and measure low concentrations of estradiol, testosterone, and LH in the serum and urine of peripubertal and pubertal children [21,22].
Gonadotropins can be measured in 24-hour urine samples obtained from healthy prepubertal children, but that method is cumbersome, requiring many technical procedures and much effort [23]. A single, nontimed measurement of urinary gonadotropin levels was reported to be effective in children because the urinary LH/FSH ratio in pubertal children is significantly higher than the serum LH/FSH ratio in prepubertal children [10]. Urinary LH/Cr ratios were also found to be higher in pubertal than prepubertal boys, but not girls, whereas urinary FSH/Cr ratios were higher in pubertal than prepubertal girls, but not boys. Those authors commented that the lack of significance for the LH/Cr ratio in girls likely reflected the random timing of the urine collection and the episodic excretion of gonadotropins [24], with urinary FSH excretion being more variable in both the prepubertal and pubertal groups. In another study of both boys and girls, urinary LH/Cr and LH/FSH ratios could be used to distinguish between children with CPP, on the one hand, and prepubertal children or those with other early pubertal disorders, on the other, whereas urinary FSH/Cr ratios contributed to the detection of gonadal failure, but not CPP [25].
Our results are consistent with those of previous studies. We found that urinary LH levels and urinary LH/FSH ratios, but not urinary FSH/Cr ratios, differed significantly between girls with CPP and those with PT. We did not evaluate Cr-adjusted urinary concentrations because that can result in over-or underestimation of urinary LH and FSH concentrations. Similar to previous studies, we found that urinary gonadotropin concentrations correlated strongly with serum gonadotropin levels without adjustment for Cr. However, urinary LH/Cr and FSH/Cr ratios did not correlate positively with their serum basal and peak levels. Singh et al. [26] demonstrated that the steroid and LH concentrations in FMV urine samples in adolescents are not significantly influenced by hydration status and might not require adjustment for Cr or specific gravity. Similarly, we found that those adjustments did not strengthen the correlations between urinary gonadotropin concentrations and their paired basal serum gonadotropin levels.
FMV urine samples are better indicators of gonadotropin excretion than random samples because they avoid nocturnal episodic variation. The use of FMV urine to monitor pubertal changes was introduced more than a decade ago [27]. Assays of LH concentration in FMV urine were found to be more sensitive in distinguishing rapid progressive PP from slow progressive PP than measurements of GnRH-stimulated gonadotropins (peak LH/FSH ratio and peak FSH level) [12]. Interestingly, urinary concentrations of bisphenol A adequately reflected the average exposure in spot urine, FMV, and 24-hour collection, suggesting that the use of single spot urine samples could reliably measure urinary bisphenol A concentrations [28].
To date, no consensus has been reached about monitoring the effects of treatment in patients with CPP, other than assessing physical changes and bone age. HPG suppression is usually evaluated by measuring GnRH-stimulated or unstimulated serum gonadotropin and sex hormone concentrations [29]. We evaluated the ability of a single random urine sample to evaluate HPG suppression in girls after GnRHa treatment. Measurements of spot urinary LH and FSH levels before and during GnRHa treatment reflected the response to HPG suppression as accurately as single measurements of serum gonadotropins levels. The LH concentration in FMV urine can also be used to monitor pubertal suppression after GnRHa treatment in patients with CPP [29]. However, in an outpatient setting, FMV urine collection is inconvenient for patients. Our strategy is more convenient and appears to be as effective as other tests.
This study had several limitations. Our sample size was small, and we did not evaluate changes in urinary gonadotropin concentrations after the girls stopped taking GnRHa.
In conclusion, this study describes a reliable and convenient method for initially screening and monitoring young patients with signs of early puberty. The single random urinary LH concentration and urinary LH/FSH ratio were strong noninvasive reflectors of a positive GnRHST result. Urinary LH and FSH levels could also be useful markers for monitoring HPG suppression during GnRHa treatment of children with CPP. Longer-term studies with more participants are needed to determine the optimal strategies and guidance for obtaining urine samples to assess hormone status in children and adolescents.
Notes
Ethical statement
These study protocols were approved by the Institutional Review Board (IRB) of Chungnam National University Hospital, Daejeon, South Korea, and written informed consent was obtained from all participating patients and their legitimate guardians (IRB No. 2020-09-095).
Conflicts of interest
No potential conflict of interest relevant to this article was reported.



