 |
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 23(2); 2018 > Article |
|
Abstract
Purpose
Methods
Results
Conclusions
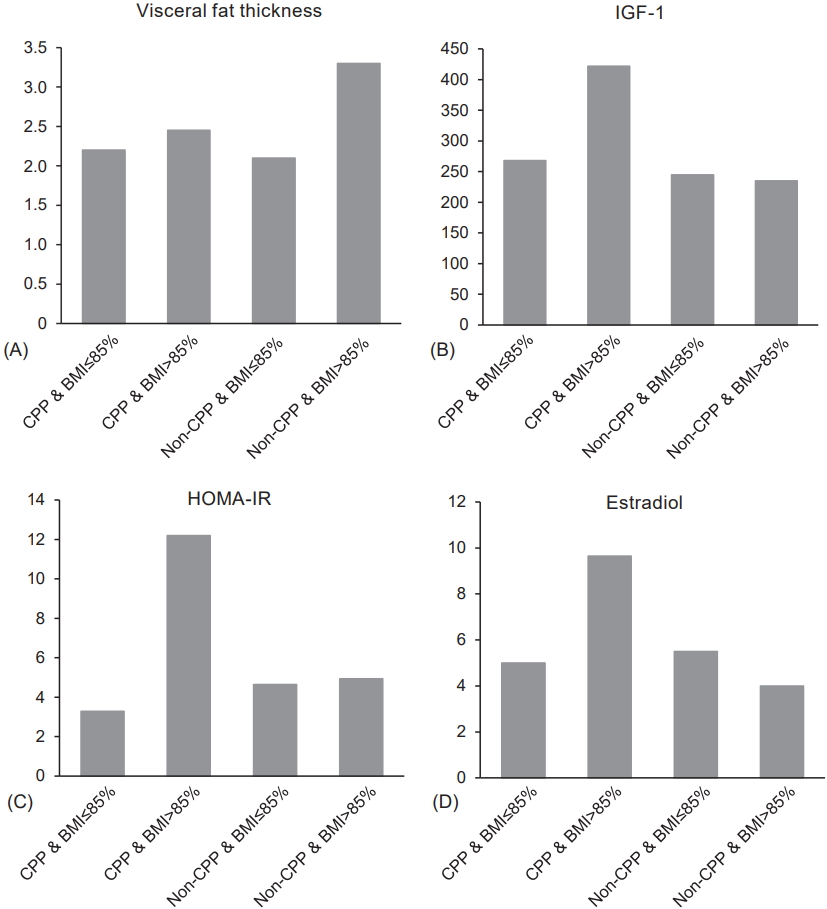
Fig.┬Ā1.
Table┬Ā1.
Values are presented as mean┬▒standard deviation.
CPP, central precocious puberty; CA, chronological age; BA, bone age; SDS, standard deviation score; BMI, body mass index; LH, luteinizing hormone; SHBG, sexual hormone binding globulin; DHEA-S, dehydroepiandrosterone sulfate; FEI, free estradiol index; IGF-1, insulin-line growth factor 1; HOMA-IR, homeostatic model assessment-insulin resistance; HDL, high-density lipoprotein; LDL, low-density lipoprotein; VFT, visceral fat thickness; SFT, subcutaneous fat thickness.
Table┬Ā2.
| Characteristic |
BMIŌēż85% |
BMI>85% |
Overall P-value | ||||
|---|---|---|---|---|---|---|---|
| Non-CPP (n=10) | CPP (n=43) | P-value | Non-CPP (n=8) | CPP (n=11) | P-value | ||
| CA (yr) | 8.5 (0.7) | 8.4 (0.7) | 0.204 | 8.3 (1.7) | 8.7 (0.7) | 0.351 | 0.441 |
| BA (yr) | 9.5 (1.0) | 9.5 (1.0) | 0.479 | 9.5 (2.0) | 11.0 (1.0) | 0.075 | 0.075 |
| BAŌĆōCA* | 1.0 (1.1) | 1.3 (1.1) | 0.138 | 1.4 (1.2) | 2.5 (1.0) | 0.062 | 0.023 |
| Weight SDS*,ŌĆĀ | 0.61 (0.82) | 0.48 (0.75) | 0.828 | 2.13 (1.04) | 1.76 (0.95) | 0.923 | <0.001 |
| BMI SDS*,ŌĆĀ | 0.59 (1.44) | 0.07 (0.63) | 0.469 | 2.05 (0.97) | 1.67 (0.69) | 0.579 | <0.001 |
| Baseline LH (IU/L)ŌĆĀ | 0.1 (0.2) | 0.6 (1.2) | <0.001 | 0.6 (0.5) | 0.8 (1.1) | 0.778 | 0.001 |
| Peak LH (IU/L) | 3.2 (2.3) | 10.3 (19.7) | <0.001 | 2.6 (2.3) | 19.1 (22.4) | <0.001 | 0.001 |
| Estradiol (pg/mL) | 5.5 (7.3) | 5.0 (20.4) | 0.620 | 4.0 (0.1) | 9.65 (42.1) | 0.033 | 0.039 |
| SHBG (nmol/L)*,ŌĆĀ | 77.3 (73.1) | 94.0 (48.9) | 0.585 | 44.5 (21.5) | 52.25 (19.5) | 0.026 | 0.001 |
| FEIŌĆĀ | 7.0 (12.0) | 6.37 (15.1) | 0.682 | 12.13 (25.0) | 24.63 (60.5) | 0.788 | 0.033 |
| Insulin (mU/L) | 20.0 (24.4) | 15.3 (31.3) | 0.856 | 19.7 (52.3) | 46.9 (47.5) | 0.600 | 0.057 |
| IGF-1 (ng/mL)* | 245 (75.0) | 268 (169.0) | 0.119 | 235 (89.0) | 422 (111.0) | <0.001 | 0.001 |
| HOMA-IR* | 4.64 (6.49) | 3.79 (8.4) | 0.838 | 4.95 (10.5) | 12.2 (10.9) | 0.545 | 0.048 |
| VFT (cm)ŌĆĀ | 2.1 (1.2) | 2.2 (0.9) | 0.964 | 3.3 (1.1) | 2.45 (0.9) | 0.016 | 0.011 |
| SFT (cm)ŌĆĀ | 0.8 (1.0) | 0.9 (0.4) | 0.991 | 1.9 (0.9) | 1.53 (0.9) | 0.152 | 0.001 |
| VFT:SFT | 2.62 (2.37) | 2.18 (1.36) | 0.964 | 2.0 (1.3) | 1.82 (2.0) | 0.778 | 0.876 |
Values are presented as median (interquartile range). Comparative analysis between groups was done with the Kruskal-Wallis test.
CPP, central precocious puberty; CA, chronologic age; BA, bone age; SDS, standard deviation score; BMI, body mass index; LH, luteinizing hormone; SHBG, sex hormone binding globulin; FEI, free estradiol index; IGF-1, insulin-like growth factor-1; HOMA-IR, homeostatic model assessment-insulin resistance; VFT, visceral fat thickness; SFT, subcutaneous fat thickness.
Table┬Ā3.
References
- TOOLS
- Related articles in APEM







