Introduction
Childhood obesity is a major public health problem around the world [
1,
2]. The prevalence of obesity in children and adolescents continues to increase worldwide, with adolescent obesity recognized as a new epidemic disease [
1,
3]. Due in part to the occurrence of the new infectious disease coronavirus disease 2019 (COVID-19), the number of obese children is steadily increasing [
2].
It is well-known that obesity is closely related to metabolic health status [
3]. Obesity causes excessive fat accumulation, leading to dyslipidemia and hypertension. Moreover, obesity increases insulin resistance, resulting in glucose intolerance and metabolic disorders [
2,
3]. Overweight children show a higher risk of becoming obese adults [
2,
4]. An increase in the unhealthy population reduces the quality of life of individuals and families and adversely affects the National Health Insurance [
5]. Abuse of diet pills and eating disorders are common problems for children and adolescents [
6].
Childhood is an important period of life for health intervention to prevent obesity development. It is common practice to eat less and move more to prevent obesity; however, the factors affecting obesity and metabolic syndromes remain controversial. Various analyses of the factors related to these changes have been attempted, but none have been definitive.
During the COVID-19 pandemic, changes in national policies, such as self-isolation and school/restaurant closures, changed everyday life. Therefore, this is a good opportunity to compare and observe the factors that affected the changes in the prevalence of obesity before and during the COVID-19 pandemic.
We aimed to identify the annual changes in the prevalence of obesity, diabetes, dyslipidemia, and hypertension before and during the COVID-19 pandemic. We also investigated lifestyleassociated factors, such as dietary habits, nutritional differences, and physical activity, which contributed to these changes before and during the COVID-19 pandemic. Through this study, we intend to investigate areas of focus in healthcare for children and adolescents and factors that can improve metabolic health.
Discussion
The results of this study revealed that the prevalence of childhood obesity and overweight continued to increase before and during the COVID-19 pandemic. The observed increase in the prevalence of overweight/obesity among Korean adolescents from 2018–2021 is consistent with previous epidemiological studies on trends in pediatric obesity [
2,
9] and reports indicating a surge in obesity among Korean children during the COVID-19 pandemic [
10].
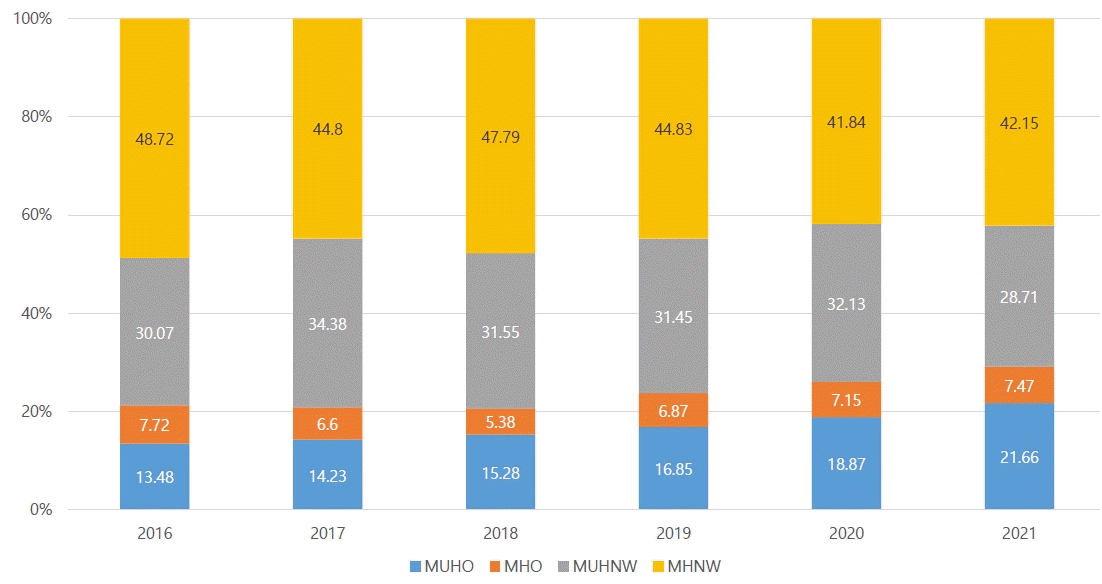
Although obesity is not always metabolically unhealthy, those classified as MHO are at risk of MUHO [
9,
11]. In 2020–2021, the prevalence of MUHO significantly increased, whereas the prevalence of MHNW decreased. Taken together, these findings indicate that Korean adolescents have become increasingly obese and unhealthy during the COVID-19 pandemic.
The prevalence of diabetes in children and adolescents is gradually increasing [
12]. When comparing metabolic factors before and during the COVID-19 pandemic, we found that obesity influenced the increasing trend in prediabetes; however, there were no significant changes in other factors except 6.5%>HbA1c≥5.7%. Most of the data used in this study was FBS (99.8% of the total). However, since postprandial hyperglycemia serves as an early indicator of insulin resistance and overweight [
13], lack of data on postprandial blood glucose level may affect the results of this study. This may explain why dysglycemia was not high in this study. In addition, considering that the definition of diabetes includes not only FBS ≥126 mg/dL and/or HbA1c ≥6.5% but also random glucose ≥200 mg/dL with symptoms and glucose level ≥200 mg/dL after a two-hour 75 g oral glucose tolerance test, the prevalence of diabetes may be underestimated.
Insulin resistance is a key factor in metabolic syndrome, and blood free fatty acids (FFA) contribute to its early development by stimulating glucose, TG, and very-low-density lipoprotein production in the liver. Our study of obese children and adolescents showed increasing TG and HbA1c levels, along with decreased HDL-C levels, which may lead to other metabolic issues. In addition, as adipose tissue increases, pro-inflammatory cytokines also rise [
14], contributing to insulin resistance. During the COVID-19 pandemic, we observed a trend of increased homeostatic model assessment for insulin resistance level >2.0 in all participants, irrespective of obesity or normal weight groups. Moreover, the prevalence of TG-glucose index ≥8.45 [
15] also increased, particularly in 2020.
Our study revealed a strong correlation between BMI and central obesity in parents and their children, especially in the elementary school aged group, as children are heavily influenced by their parents. During the COVID-19 pandemic, as the frequency of eating with family members increased, the influence of families on their children strengthened. Previous studies have shown that children with overweight/obese parents exhibited unhealthy dietary and lifestyle habits [
16], wherein the higher was the mother's BMI, the higher was the child's BMI.
Moreover, physical activity decreased, leading to longer periods of sitting [
17]. Unhealthy BMI in children has also been associated with increased screen use5 [
18], and reduced fruit consumption [
19]. These findings support the notion that parental BMI reflects health habits, which affect the child's health habits and weight status [
20]. Therefore, family counseling is thought to be more effective to treat obese children, and a family centered healthy life, including diet and physical activity, should be emphasized, especially in younger children. However, this correlation was not significant in the middle school and high school aged groups, possibly because the influence of parents on their children's behavior decreased as the children matured and became more independent [
21]. Furthermore, school programs [
22] and peer [
23] influence can also affect behavior and BMI status in older children. Therefore, adolescents may require a distinct approach that encompasses a wider range of aspects.
It is well-known that reduced fruit and vegetable intake leads to obesity [
2,
19]. Kim et al. [
24] reported a decrease in fruit intake among 12–18-year-olds during the COVID-19 pandemic; however, our study did not identify any significant changes in the intake of fiber or vitamins, which are abundant in these foods. It was confirmed that the intake of niacin, folic acid, and vitamin C was lower than the recommended intake presented in the Dietary Reference Intakes for Koreans in 2020 [
8] among middle and high school students. Since niacin is known to inhibit TG synthesis and reduce HDL-apoA-I catabolism, reduced niacin intake may play a role in the increasing dyslipidemia in children and adolescents. Folic acid level showed a significant positive correlation with HDL-C and a significant negative correlation with TG [
25]. Thiamine is an essential trace element for glucose metabolism, and doubling the daily thiamine intake was significantly associated with a 7% reduction in metabolic syndrome among adults with comorbidities [
26]. Folic acid supplementation could protect against obesity and prevent obesity-related complications, such as insulin resistance, and cardiovascular and metabolic disorders [
27]. Vitamin C has an antioxidant effect that removes free radicals, which can play a role in improving vascular endothelial dysfunction caused by increased free radicals, owing to paracrine effects in the adipose tissue [
28]. Therefore, reduced fruit and vegetable intake may have been responsible for the increased prevalence of obesity during the COVID-19 pandemic due to the reduced intake of vitamins. However, excessive vitamin B intake may contribute to obesity [
29], and high-dose vitamin C does not improve endothelial dysfunction or insulin resistance [
30], and further research is needed into the link between reduced trace element intake and obesity.
According to a previous meta-analysis, skipping breakfast increases the risk of overweight/obesity [
31], and adolescents who regularly eat breakfast have lower body fat [
32]. We discovered that the proportion of people who skipped breakfast increased during the COVID-19 pandemic, particularly in the obese group. There are several reasons that skipping breakfast can lead to obesity. Eating breakfast can positively impact obesity by disrupting long-term fasting, regulating glucose homoeostasis and insulin sensitivity [
33] and enabling greater physical activity thermogenesis in the morning [
34]. While breakfast helps maintain more stable afternoon and evening glycemia than fasting, skipping breakfast leads to increased postprandial hyperglycemia after lunch and dinner [
34], which is associated with insulin resistance, leading to obesity. Postprandial hyperglycemia and insulin resistance can result in increased food intake by increasing insulin and FFA levels and hunger and decreasing satiety [
35]. Previous studies have shown conflicting findings on the association between skipping breakfast and overweight [
36], with some suggesting that skipping dinner, not breakfast, may be a predictor of weight gain and overweight/obesity [
37]. However, based on our results, it can be inferred that the social influence of COVID-19 affected the frequency of eating breakfast and the occurrence of pediatric obesity. Therefore, additional research is necessary to clearly understand the mechanisms underlying the correlations between eating habits and physiological changes.
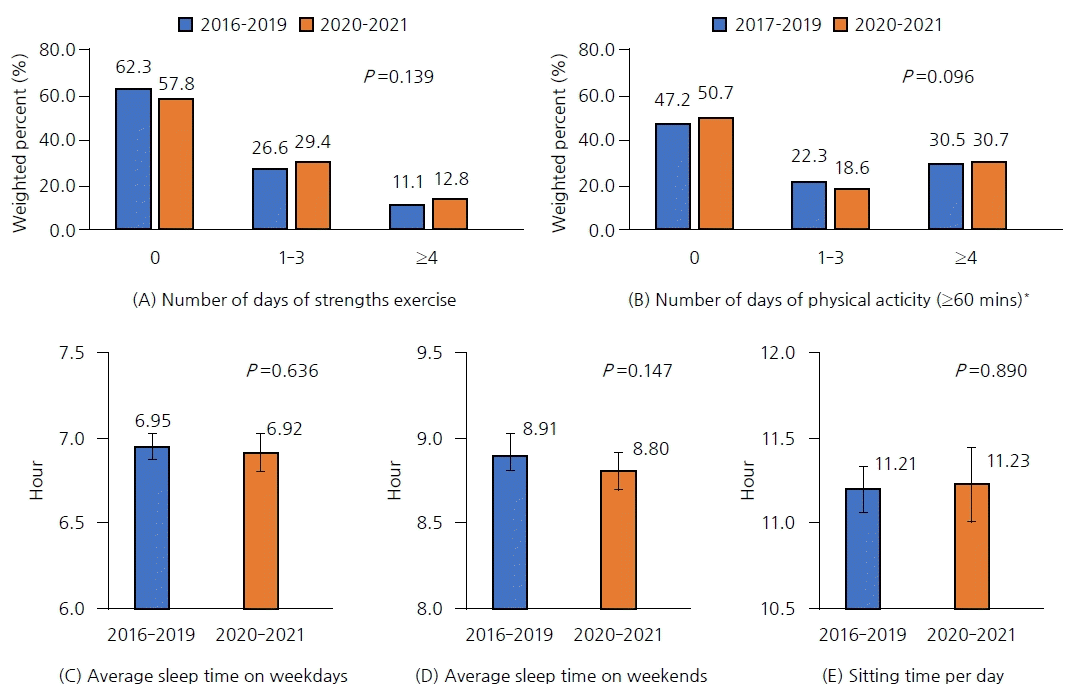
Changes in physical activity duration did not decrease significantly in our study, which is presumed to be due to the limited availability of detailed physical activity data for KNHANES. However, in a 2019–2020 comparative study using the Adolescent Health Behavior Survey [
10], sleep time decreased and inactivity increased. Many other studies have also reported a correlation between lifestyle habits such as sedentary behavior or screen time [
5,
18] and obesity.
Although this study was conducted using nationwide survey data, it had some limitations. First, the cross-sectional data only allowed evaluation of changes in prevalence and associations among parents; hence, it remains unknown which group was reclassified into MUHO based on annual changes in health status in the same person, and evaluation of long-term child health status was not possible. Second, a fixed cut-off of 130/85 mmHg was applied to the criteria for high BP regardless of age, gender, and height. Third, during the COVID-19 pandemic, social restrictions led to increased food consumption through delivery or take-out. Without consideration of these details, the evaluation of eating habits and food quality before and during the pandemic may not be accurate.
Nevertheless, this study has the strengths of being a multifaceted study of obesity and metabolic syndrome-related indicators in a special COVID-19 environment. Metabolic diseases are not simply caused or controlled by a single factor but are complex phenomena that occur through various mechanisms. This study was meaningful since it investigated factors across age, sex, socioeconomic status, physical activity, lifestyle, parental health status, nutrition, and dietary habits.
In conclusion, obesity in children and adolescents is sensitive to the social environment, and MUHO increased during the COVID-19 pandemic. Attention should be paid during childhood to improve children's health indicators. Agespecific strategies that consider growth, development, and genetic and social factors are required. Furthermore, health strategies targeting the entire family are required to develop healthier habits to ensure that overweight/obesity or unhealthy behaviors are not passed on from parents to offspring. Efforts toward developing healthy habits will ultimately help improve children's health. Further longitudinal studies are needed to explore factors associated with metabolic health and long-term outcomes.