A baby with congenital hypothyroidism born to a hypothyroid mother who expressed undiagnosed thyroid stimulation blocking antibody
Article information
Abstract
In adults, hypothyroidism caused by thyroid stimulation blocking antibody (TSB Ab) is rare, and confirmed cases are even fewer, as TSB Ab levels are rarely assayed. However, this may create problems in babies, as the transplacental passage of maternal TSB Ab can cause a rare type of hypothyroidism in the infant. Prompt levothyroxine replacement for the baby starting immediately after birth is important. We describe a congenital hypothyroid baby born to a hypothyroid mother who was not aware of the cause of her hypothyroid condition, which turned out to be associated with the expression of TSB Ab. This cause was confirmed in both the infant and mother using a series of thyroid function tests and measurements of autoantibody levels, including TSB Ab. During periodic follow-up, the TSB Ab and thyroid stimulating hormone receptor antibody titers became negative in the baby at 8 months of age, but remained positive in the mother. Evaluation of hypothyroidism and its cause in mothers during pregnancy is important for both maternal and child health.
Introduction
Thyroid stimulating antibody (TS Ab) and thyroid stimulation blocking antibody (TSB Ab) are 2 types of thyrotropin receptor autoantibodies (TSH receptor Abs). TS Ab appears to bind the N-terminal portion of the extracellular domain and mimic the actions of thyroid stimulating hormone (TSH) by inducing postreceptor signal transduction and cell stimulation. In contrast, the C-terminal region is more important for TSB Ab which blocks stimulation by either TS Ab or TSH, causing hypothyroidism12345). TSH receptor Ab can pass through the placenta and affect the fetal thyroid hormone balance, causing neonatal hypothyroidism67). Here, we describe a congenitally hypothyroid baby born to a hypothyroid mother who was not aware that she expressed TSB Ab.
Case Report
A baby was transferred to Konkuk University Medical Center with a high TSH (117 µIU/mL) and a low free T4 (0.2 ng/dL) level revealed by neonatal screening tests performed 3 days after birth. The baby had been born vaginally at 41+1 weeks of gestation at a birth weight of 3.48 kg. In terms of family history, the mother had been diagnosed with hypothyroidism 2.5 years prior, and she took daily Synthroid. The cause of her hypothyroidism had never been explored. On physical examination, no characteristic of hypothyroidism was evident in the baby or mother.
On the initial thyroid function test (TFT), the baby had normal T3 (0.661 ng/mL; normal range, 0.62–2.43 ng/mL), low free T4 (0.269 ng/dL; normal range, 0.83–3.09 ng/dL), and high TSH (100 µIU/mL; normal range, 0.43–16.1 µIU/mL) levels. Tests for antithyroid Abs showed that the TSH receptor Ab level was >40.00 IU/L (normal, <1.75 IU/L), the antithyroid peroxidase (TPO) Ab (antimicrosomal Ab) level was >600 IU/mL (normal, <34 IU/mL), and the antithyroglobulin Ab level was >4,000 IU/mL (normal, <115 IU/mL).
The mother's TFT revealed normal T3 (1.52 ng/mL; normal range, 0.8–2.0 ng/mL), high T4 (2.57 ng/dL; normal range, 0.93–1.7 ng/dL), and low TSH (0.032 µIU/mL; normal range, 0.27–4.2 µIU/mL) levels. Tests for antithyroid Abs showed that the TSH receptor Ab level was >40.00 IU/L (normal, <1.75 IU/L), the anti-TPO Ab level was >600 IU/mL (normal, <34 IU/mL), and the antithyroglobulin Ab level was >4,000 IU/mL (normal, <115 IU/mL).
As TSH receptor Ab is expressed in some cases of hypothyroidism, we measured the TSB Ab and TS Ab titers. The infant's TSB Ab score was 97.9% (normal, <45.6%), but the TS Ab status was negative (99%; normal, <140%). The mother's TSB Ab score was 97.6% (normal, <45.6%), but the TS Ab status was negative (96.8%; normal, <140%). Therefore, the mother was confirmed to have hypothyroidism caused by TSB Ab.
Thyroid ultrasound and a sodium pertechnetate 99m thyroid scan were used to evaluate the baby. The ultrasound scan was normal. No obvious radioactivity was detected in either thyroid lobe on the Tc99m thyroid scan. Thus, the infant was diagnosed with congenital hypothyroidism attributable to TSB Ab that had passed through the placenta. The baby was started on levothyroxine (13.9 µg/kg).
The baby underwent repeat antithyroid Ab assessment and TFTs while taking levothyroxine over 10 months (Table 1, Fig. 1). The hypothyroidism was well managed by the drug (T3, 1.75 ng/mL; free T4, 1.58 ng/dL; and TSH, 2.22 µIU/mL), and the TSH receptor Abs became washed out (TSH receptor Ab, 0.46 IU/L; TSB Ab, 0%). In contrast, the mother's findings did not change over the 8 months (TSH receptor Ab, >40.00 IU/L; TSB Ab, 101.0%; and figures in the high-normal ranges for anti-TPO Ab and anti-thyroglobulin Ab) (Fig. 1).
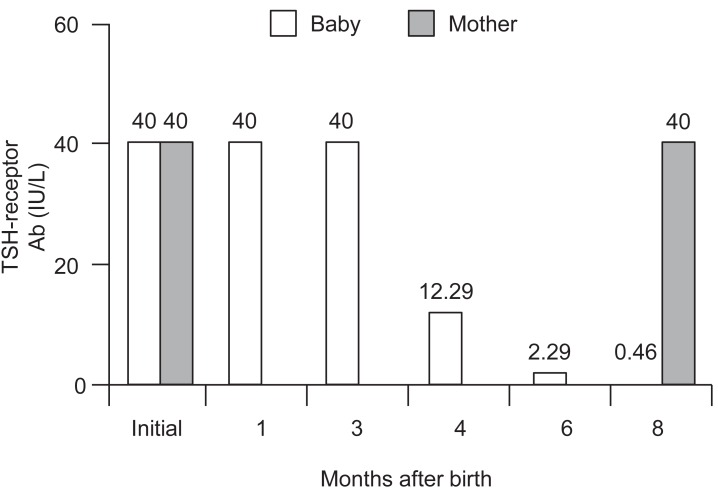
Serum thyroid stimulating hormone (TSH) receptor titers of the mother and baby at various times after birth. Ab, antibody.
The baby was diagnosed with transient congenital hypothyroidism caused by TSB Ab transferred through the placenta. The baby is now taking 30 µg/day levothyroxine (3.2 µg/kg); we plan to review the dose after additional follow-up testing.
Discussion
We described a baby with transient congenital hypothyroidism born to a mother who was not known the cause of her hypothyroidism. TSB Ab-associated congenital hypothyroidism, which constitutes 1%–2% of all cases of congenital hypothyroidism, is usually observed in babies whose mothers are taking T4, have undiagnosed hypothyroidism, or have a history of autoimmune hypothyroidism89). TSB Ab triggers hypothyroidism by inhibiting the TSH-induced production of cyclic adenosine monophosphate, iodide uptake, and thyroglobulin synthesis.
In adult hypothyroid patients with autoimmune thyroiditis, hypothyroidism attributable to TSB Ab is uncommon (15% of patients)10). As measurement of TSH receptor Ab levels is considered appropriate only in patients with Graves' disease, such tests are recommended only if a pregnant woman has a history of Graves' disease, not hypothyroidism1112). For this reason, it is difficult to define the cause of hypothyroidism caused by TSB Ab. In this situation, transplacental passage of TSB Ab can cause neonatal hypothyroidism in a pregnant patient.
Although almost all babies with neonatal hypothyroidism exhibit no symptoms at birth, thyroid function in the neonate is influenced by maternal Abs13). And switching between TSB Ab and TS Ab can unusually occur in patients who are under levothyroxine therapy for hypothyroidism and who experience immunosuppression and/or hemodilution during pregnancy. Such switching usually reduces thyroid autoantibody levels14). TSH receptor Ab status should be examined when the cause of neonatal and maternal hypothyroidism is uncertain7).
Although several cases about TSB Ab-associated congenital hypothyroidism have been reported, screening about TSH receptor Ab is still seldom tested in adult. And almost all clinicians have focused on only treatment of hypothyroidism or hyperthyroidism regardless of the presence of TSH receptor Ab in baby and adult. However, it should be borne in mind that a hypothyroid baby born to a mother with hypothyroidism attributable to TSB Ab may have severe neonatal hypothyroidism. Therefore a testing for TSB Ab in adults with hypothyroidism with TSH receptor Ab is required. Especially in pregnant mothers TSB Ab should be assayed; this is important in terms of both maternal and child health.
Notes
Conflict of interest: No potential conflict of interest relevant to this article was reported.
