 |
 |
- Search
| Ann Pediatr Endocrinol Metab > Volume 20(1); 2015 > Article |
|
Abstract
Purpose
Methods
Results
Conclusion
References
Fig.┬Ā1
Schematic representation of diabetic patients with persistent, regression, and progression groups to microalbuminuria. T1DM, type 1 diabetes mellitus; T2DM, type 2 diabetes mellitus.
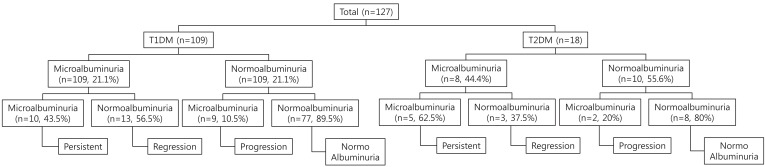
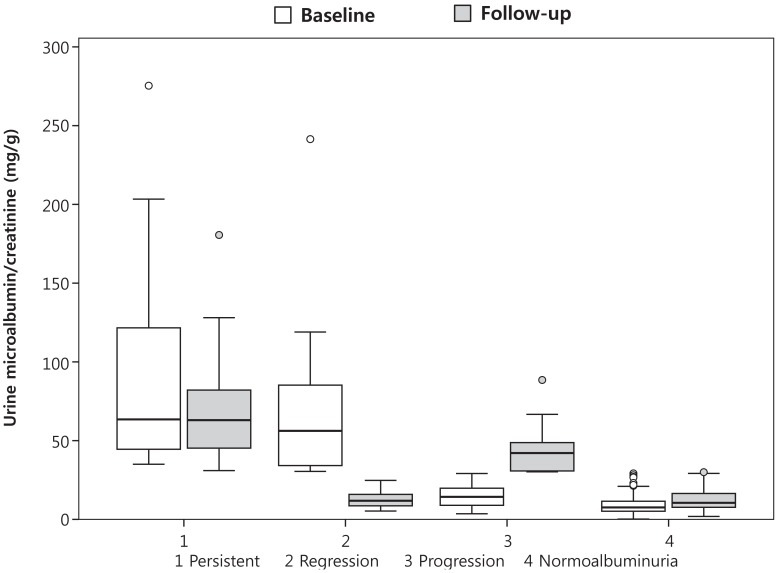
Fig.┬Ā2
Comparison of spot urine microalbumin/creatinine ratio between baseline and follow-up assessment. The median is depicted by the horizontal line, the interquartile range by the box limits, ranges by the whiskers, and outliers by the circles.
Table┬Ā1.
Anthropometric and laboratory characteristics of patients with type 1 and type 2 diabetes
| Variable |
T1DM (n=109) |
T2DM (n=18) |
||
|---|---|---|---|---|
| Baseline | Follow-up | Baseline | Follow-up | |
| Anthropometric index | ||||
| ŌĆāAge (yr) | 17.5a)(15.1ŌĆō20.5) | 18.9 (16.5ŌĆō21.0) | 15.4a)(12.6ŌĆō17.4) | 17.9 (16.8ŌĆō18.4) |
| ŌĆāSex, male/female | 39/70 | 4/14 | ||
| ŌĆāDiabetes duration (yr) | 9.5a)(6.5ŌĆō13.5) | 10.1 (7.8ŌĆō14.0) | 0.9a)(0.0ŌĆō3.0) | 5.0 (3.5ŌĆō5.6) |
| ŌĆāHeight (cm) | 162.0a)(160.0ŌĆō170.0) | 162.9 (160.0ŌĆō172.0) | 158.5a)(153.5ŌĆō160.5) | 160.2 (153.5ŌĆō163.2) |
| ŌĆāWeight (kg) | 57.0a)(53.0ŌĆō64.0) | 58.5 (54.0ŌĆō65.0) | 61.0 (54.0ŌĆō73.7) | 63.4 (54.0ŌĆō75.5) |
| ŌĆāBMI (kg/m2) | 21.52a)(19.53ŌĆō23.15) | 21.91 (20.03ŌĆō23.41) | 24.74 (21.09ŌĆō30.88) | 24.31 (21.09ŌĆō29.02) |
| ŌĆāHeight z-score | 0.12a)(ŌĆō0.44 to 1.19) | 0.05 (ŌĆō0.55 to 0.86) | 0.50a)(ŌĆō0.15 to 0.71) | ŌĆō0.10 (ŌĆō1.45 to 0.13) |
| ŌĆāWeight z-score | 0.31 (ŌĆō0.17 to 1.00) | 0.27 (ŌĆō0.17 to 1.02) | 1.02a)(ŌĆō0.01 to 2.50) | 0.35 (ŌĆō0.01 to 2.17) |
| ŌĆāBMI z-score | 0.31 (ŌĆō0.43 to 0.78) | 0.30 (ŌĆō0.43 to 0.83) | 1.29 (ŌĆō0.02 to 2.49) | 0.99 (ŌĆō0.01 to 2.27) |
| Biochemical profiles | ||||
| ŌĆāSerum creatinine (mg/dL) | 0.80 (0.70ŌĆō0.90) | 0.75 (0.69ŌĆō0.85) | 0.80 (0.60ŌĆō0.90) | 0.65 (0.60ŌĆō0.76) |
| ŌĆāeGFR (mL/min/1.73 m2) | 125.7 (110.0ŌĆō134.6) | 127.9a)(118.8ŌĆō136.1) | 128.5 (109.9ŌĆō156.3) | 139.6 (129.0ŌĆō152.1) |
| ŌĆāUrine microalbumin/creatinine (mg/g) | 9.4 (6.3ŌĆō26.6) | 13.3 (8.6ŌĆō24.8) | 25.3 (11.5ŌĆō56.0) | 17.7 (6.2ŌĆō42.0) |
| ŌĆāCholesterol (mg/dL) | 175.0 (167.0ŌĆō230.0) | 179.0 (163.0ŌĆō206.0) | 194.0 (161.0ŌĆō231.0) | 150.0 (139.0ŌĆō222.0) |
| ŌĆāTG (mg/dL) | 79.0 (61.0ŌĆō101.0) | 74.0 (56.0ŌĆō93.0) | 105.0 (85.0ŌĆō235.0) | 92.0 (64.0ŌĆō262.0) |
| ŌĆāHDL-cholesterol (mg/dL) | 58.0 (50.0ŌĆō68.0) | 60.0a)(52.0ŌĆō68.0) | 49.5 (43.0ŌĆō52.0) | 53.0 (45.0ŌĆō59.0) |
| ŌĆāHbA1c (%) | 8.3 (7.3ŌĆō9.6) | 8.4 (7.4ŌĆō9.6) | 8.8 (6.9ŌĆō12.2) | 7.8 (6.2ŌĆō11.7) |
| ŌĆāC-peptide (ng/mL) | 0.02 (0.015ŌĆō0.039) | 0.02 (0.015ŌĆō0.018) | 2.97a)(2.471ŌĆō3.733) | 1.96 (1.432ŌĆō2.393) |
Values are presented as median (interquartile range) or number.
T1DM, type 1 diabetes mellitus; T2DM, type 2 diabetes mellitus; BMI, body mass index; eGFR, estimated glomerular filtration rate; TG, triglyceride; HDL-cholesterol, high density lipoprotein cholesterol; HbA1c, glycosylated hemoglobin; C-peptide, connecting peptide.
Table┬Ā2.
Characteristics of patients with type 1 diabetes according to microalbuminuria status (n=109)
| Characteristic |
Persistent (n=10) |
Regression (n=13) |
Progression (n=9) |
Normal (n=77) |
||||
|---|---|---|---|---|---|---|---|---|
| Baseline | Follow-up | Baseline | Follow-up | Baseline | Follow-up | Baseline | Follow-up | |
| Anthropometric index | ||||||||
| ŌĆāAge (yr) | 17.8 (14.5-22.5) | 19.2 (17.0-23.0) | 17.0 (15.0-21.0) | 20.0 (17.5-21.5) | 19.0 (19.0-24.5) | 20.0 (19.5-25.0) | 17.5 (15.0-20.5) | 18.0 (15.5-21.0) |
| ŌĆāSex, male/female | 2/8 | 4/9 | 3/6 | 4/9 | ||||
| ŌĆāDiabetes duration (yr) | 12.0 (7.5-16.0) | 12.8 (8.0-16.5) | 10.0 (5.0-11.1) | 10.5 (7.9-13.0) | 11.5 (5.5-15.0) | 12.0 (7.5-16.0) | 9.5 (6.5-13.5) | 10.0 (7.0-14.0) |
| ŌĆāFollow-up duration (yr) | 0.5 (0.5-1.0)a) | 1.0 (0.5-4.0) | 0.5 (0.5ŌĆō1.0)b) | 1.0 (0.5-0.5) | ||||
| ŌĆāHeight z-score | 0.10 (-0.15-0.63) | 0.11 (-0.15 to 0.53) | -0.15 (-0.41 to 0.28) | -0.22 (-0.55 to 0.26) | 0.01 (-0.15 to 0.25) | -0.01 (-0.15 to 0.25) | 0.24 (-0.55 to 1.02) | 0.15 (-0.55 to 0.86) |
| ŌĆāWeight z-score | 0.67 (0.32-1.13) | 0.68 (0.04-1.02) | 0.42 (-0.10-0.71) | 0.22 (-0.09 to 1.13) | 0.08 (-0.02 to 0.79) | 0.08 (-0.02 to 0.79) | 0.29 (-0.17 to 0.90) | 0.29 (-0.17 to 0.90) |
| ŌĆāBMI z-score | 0.55 (0.28-0.83) | 0.51 (0.12-0.83) | 0.39 (-0.12 to 0.76) | 0.34 (0.30-0.68) | -0.04 (-0.47 to 0.77) | -0.04 (-0.11 to 0.77) | 0.28 (-0.50 to 0.59) | 0.25 (-0.50 to 0.59) |
| Biochemical profiles | ||||||||
| ŌĆāsCr (mg/dL) | 0.70 (0.60-0.90) | 0.69 (0.65-0.74) | 0.80 (0.70-1.00) | 0.73 (0.69-0.99) | 0.78 (0.60-0.80) | 0.75 (0.74-0.81) | 0.80 (0.70-0.90) | 0.76 (0.69-0.86) |
| ŌĆāeGFR (mL/min/1.73 m2) | 127.7 (110.0-165.0) | 129.5 (125.3-156.6) | 116.3 (99.4-127.3) | 128.3 (119.3-135.4) | 117.3 (116.9-148.5) | 118.8 (116.5-128.8) | 125.7 (110.0-133.6) | 127.5 (117.0-136.1) |
| ŌĆāUrine microalbumin/creatinine (mg/g) | 63.3 (48.9-171.8) | 58.0 (48.0-92.4) | 56.4 (34.1-74.0) | 9.6 (8.6-15.8) | 15.4 (11.4-22.0) | 42.1 (30.8-50.2) | 7.4 (5.0-10.1) | 11.3 (7.8-16.5) |
| ŌĆāCholesterol (mg/dL) | NA | NA | 175.0 (160.0-214.0) | 168.0 (163.0-206.0) | NA | NA | 181.0 (175.0-187.0) | 177.5 (160.0-195.0) |
| ŌĆāTG (mg/dL) | 70.0 (64.0-135.0) | 75.0 (68.0-119.0) | 79.5 (67.0-109.0) | 77.5 (73-94) | 92.0 (81-94) | 71.0 (61-89) | 76.0 (56-99) | 67.0 (53-91) |
| ŌĆāHDL-cholesterol (mg/dL) | 58.0 (56.0-64.0) | 55.0 (53.0-66.0) | 58.0 (53.0-67.0) | 61.5 (55.0-68.0) | 56.0 (45.0-68.0) | 60.0 (47.0-75.0) | 58.0 (49.0-67.0) | 60.0 (52.0-68.0) |
| ŌĆāHbA1c (%) | 9.8 (8.7-13.8)c) | 9.7 (8.9-10.1)d) | 8.0 (7.0-8.9)e) | 8.0 (7.1-9.4)f) | 9.6 (8.5-10.2) | 9.5 (7.8-10.1) | 8.2 (7.1-9.1) | 8.1 (7.2-9.0) |
| ŌĆāC-peptide (ng/mL) | 0.02 (0.015-0.015) | 0.02 (0.015-0.018) | 0.27 (0.015-0.571)g) | 0.02 (0.020-0.050) | 0.03 (0.015-0.100)h) | 0.04 (0.020-0.092) | 0.02 (0.015-0.020) | 0.02 (0.015-0.022) |
Values are presented as median (interquartile range or range) or number.
T1DM, type 1 diabetes mellitus; BMI, body mass index; sCr, serum creatinine; eGFR, estimated glomerular filtration rate; TG, triglyceride; HDL-cholesterol, high density lipoprotein cholesterol; HbA1c, glycosylated hemoglobin; C-peptide, connecting peptide; NA, not available.
Table┬Ā3.
Characteristics of patients with type 2 diabetes according to microalbuminuria status (n=18)
| Characteristic |
Persistent (n=5) |
Regression (n=3) |
Progression (n=2) |
Normoalbuminuria (n=8) |
||||
|---|---|---|---|---|---|---|---|---|
| Baseline | Follow-up | Baseline | Follow-up | Baseline | Follow-up | Baseline | Follow-up | |
| Anthropometric index | ||||||||
| ŌĆāAge (yr) | 14.9 (13.3-16.8) | 17.9 (17.8-18.1) | 14.1 (11.9-26.0) | 18.2 (13.8-27.0) | 18.9 (15.8-22.0) | 19.7 (16.8-22.5) | 14.4 (12.3-17.4) | 17.0 (15.8-18.4) |
| ŌĆāSex, male/female | 0/3 | 0/5 | 0/2 | 4/4 | ||||
| ŌĆāDiabetes duration (yr) | 2.6 (0.2-3.0) | 5.6 (5.3-6.6) | 0.0 (0.0-13.0) | 4.1 (1.9-14.0) | 2.3 (0.5-4.0) | 3.0 (1.0-5.0) | 0.7 (0.0-3.0) | 4.6 (3.2-5.1) |
| ŌĆāFollow-up duration (yr) | 4.4 (3.0-5.1) | 1.9 (1.0-4.1) | 0.8 (0.5-1.0) | 2.6 (0.5-5.0) | ||||
| ŌĆāHeight z-score | 0.00 (-0.02 to 0.01)a) | -0.02 (-1.45 to -0.01) | -0.15 (-0.55 to 0.05) | -0.63 (-0.79 to -0.15) | -1.92 (-2.23 to -1.60) | -1.92 (-2.23 to -1.61) | 0.65 (0.46-0.98) | 0.12 (-0.70 to 0.47) |
| ŌĆāWeight z-score | 2.33 (1.18-2.50) | 1.56 (1.47-2.38) | -0.15 (-2.16 to -0.02) | -0.02 (-3.07-0.04) | 0.20 (0.13-0.27) | 0.20 (0.13-0.27) | 1.74 (0.31-2.68) | 0.63 (-0.01 to 2.29) |
| ŌĆāBMI z-score | 2.10 (1.28-2.85) | 2.27 (1.57-2.35) | -0.26 (-2.39 to -0.02) | -0.02 (-2.97 to 0.49) | 1.16 (1.00-1.31) | 1.13 (0.94-1.31) | 1.83 (-0.07 to 2.57) | 0.99 (-0.16 to 2.27) |
| Biochemical profiles | ||||||||
| ŌĆāsCr (mg/dL) | 0.80 (0.58-0.90) | 0.59 (0.49-0.64) | 0.80 (0.52-1.10) | 0.62 (0.55-0.76) | 0.63 (0.60-0.65) | 0.71 (0.66-0.76) | 0.85 (0.65-0.90) | 0.75 (0.61-0.81) |
| ŌĆāeGFR (mL/min/1.73 m2) | 110.3 (99.3-151.9) | 152.1 (131.8-180.4) | 115.8 (77.5-158.7) | 136.2 (110.0-157.5) | 132.9 (128.2-137.5) | 117.7 (108.6-126.8) | 131.3 (109.9-181.5) | 145.2 (131.1-148.6) |
| ŌĆāUrine microalbumin/creatinine (mg/g) | 63.48 (40.18-117.46) | 68.59 (42.04-72.26) | 56.00 (34.29-241.43) | 15.29 (13.23-20.02) | 6.21 (3.55-8.88) | 38.76 (30.20-47.32) | 13.16 (9.29-21.32) | 5.96 (3.83-9.13) |
| ŌĆāCholesterol (mg/dL) | 218.0 (194-253) | 209.0 (147-338) | 196.0 (161-231) | 174.0 (160-188) | NA | NA | 162.0 (136-165) | 139.0 (136-141) |
| ŌĆāTG (mg/dL) | 295.0 (179-581)b) | 326.0 (320-572)c) | 87.0 (85-251) | 95.0 (60-149) | 181.0 (127-235) | 215.0 (168-262) | 68.5 (55-106) | 64.0 (60-82) |
| ŌĆāHDL-cholesterol (mg/dL) | 52.0 (51-52) | 54.0 (45-57) | 64.0 (41-73) | 59.0 (44-64) | 39.5 (35-44) | 43.5 (41-46) | 47.5 (43-50) | 53.0 (45-66) |
| ŌĆāHbA1c (%) | 11.2 (7.0-12.2) | 11.1 (8.2-12.3) | 13.3 (7.6-15.0) | 6.3 (6.1-12.1) | 6.7 (6.1-7.3) | 7.8 (6.4-9.2) | 8.3 (5.6-11.1) | 6.6 (5.4-11.7) |
| ŌĆāC-peptide (ng/mL) | 3.73 (2.710-3.750) | 2.25 (1.960-3.100) | 2.08 (1.010-2.230) | 2.43 (1.420-3.440) | 3.41 (2.470-4.340) | 1.83 (1.270-2.390) | 3.00 (2.970-3.200) | 1.63 (1.180-2.130) |
Values are presented as median (interquartile range or range) or number.
T2DM, type 2 diabetes mellitus; BMI, body mass index; sCr, serum creatinine; eGFR, estimated glomerular filtration rate; TG, triglyceride; HDL-cholesterol, high density lipoprotein cholesterol; HbA1c, glycosylated hemoglobin; C-peptide, connecting peptide; NA, not available.
- TOOLS
-
METRICS

-
- 8 Crossref
- Scopus
- 9,788 View
- 138 Download





